Venous Ulcers
Venous ulcers can develop when the circulation in your legs and feet slows down and interferes with your body’s ability to heal itself. If you have any of these deep open wounds, expert vascular surgeon Dennis Resetarits, MD, of Surgical Care East, PLLC in Camillus, New York, can help. Dr. Resetarits and his team use the latest methods to treat venous ulcers and address the vein diseases that cause them. Call Surgical Care East, PLLC to find out more or book an appointment online today.
What are venous ulcers?
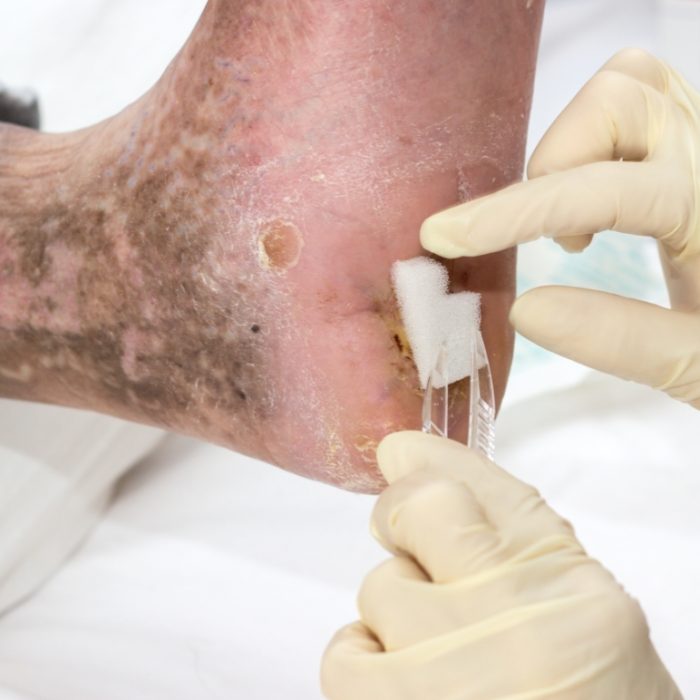
Venous ulcers are wounds or sores on your skin that tend to develop on your legs, particularly around your ankles. Some are shallow, but many form deep wounds that can be extremely painful.
Venous ulcers often prove resistant to healing, meaning they may stay open for months and sometimes years. This can have a significant adverse effect on your quality of life, and infected wounds can sometimes lead to bone infections and tissue death (gangrene).
In the worst cases, complications like these may result in the need for amputation to prevent the infection from spreading to the rest of your body, which could prove fatal.
Don’t allow your vascular conditions to progress. Visit us to have our expert team evaluate your condition to stop the progression of vein disease.
What causes venous ulcers?
Venous ulcers are a consequence of reduced circulation in your veins (venous stasis). Your legs are particularly vulnerable to venous stasis because while they’re trying to push blood up and back to your heart, gravity is dragging it down toward your feet.
Vein diseases like venous insufficiency make this problem worse. Weakened valves in the veins allow blood to trickle backward, where it pools and forms varicose veins. As the veins worsen, fluid seeps into the surrounding tissues.
To make matters worse, having poor circulation means there’s a lack of oxygen and nutrients in the tissues. This affects your immune system and stops your body from repairing itself properly. Toxins also build up, inflammation sets in, and the tissues start to deteriorate.
Any minor break in the skin at this point can lead to a venous ulcer. You’re more likely to get venous ulcers if you have diabetic peripheral neuropathy — a common complication of diabetes that causes numbness in your feet, meaning you might be unaware of minor wounds.
How are venous leg ulcers treated?
There are two aspects to treating venous ulcers. One is to clean and dress the wound; the other is to address the underlying cause.
Wound care is a specialized area of vein care. It involves the removal of dead or infected tissue from the ulcer, a process known as debridement. There are various methods of performing debridement, including surgery.
Once the wound has no dead tissue left, the Surgical Care East, PLLC team cleans it thoroughly and applies a dressing to protect it and help it heal.
Treating the underlying cause of your venous ulcer involves improving the circulation in your leg. Dr. Resetarits achieves this by performing a minimally invasive procedure to destroy or remove diseased veins. Options include:
- Asclera® sclerotherapy
- VenaSeal™ vein closure system
- ClosureFast™ endovenous radiofrequency ablation
- Ambulatory (microhook) phlebectomy
To benefit from the expertise of the Surgical Care East, PLLC team in managing venous ulcers, call their office today or book an appointment online. Now serving Camillus, NY, and surrounding areas of Syracuse.
